Blog
Hospitals will receive $ 1.7 billion more federal financing. Will this shorten the waiting time?
This week, the federal government announced He will pay additional, one -off, $ 1.7 billion for public hospitals for countries and territories.
This was charged as a way to repair the ailing hospitals and shortening the waiting for care in emergency departments and surgery to choose from. But will it really make a difference?
How are hospitals financed?
Australian public hospitals are financed from a cooperation agreement with the participation of state governments, territory and federal. The federal government ensures 37% of the financing of a public hospital annually, mainly by National health reform agreement. States and territories finance almost all the rest.
Most of the federal government financing for public hospitals is determined by “Financing based on activity“Formula. Financing is based on the number of patients treated and the price of treatment, the latter calculated on the basis of the average costs of a public hospital.
State governments and territory manage public hospitals. The federal government has nothing to say about spending money from a public hospital. The exception is that financing concerns something specific, such as the recent hospital ward.
As he compares additional financing
The federal government will issue $ 30.19 billion in public hospitals This year’s financial year. Additional financing will escalate expenses for a public hospital by 12% in 2025–26.
Additional funds will probably affect hospitals in northern territory. He will receive $ 51 million more, which is an escalate of 30%.
While larger states will receive additional funds, they have more public hospitals and patients. For example, the recent southern Wales will receive $ 407 million, but this corresponds to only 11% growth of the federal government.
Additional financing is less impressive compared to total hospital expenses. It was $ 86 billion In the years 2022–23 he suggests that an additional $ 1.7 billion will represent less than 2% of additional total funds for public hospitals in 2025–26.
But these additional expenses are not in insulation. The federal government has already done this has committed almost $ 600 million establish 87 Clinics of urgent care Around Australia. Their main goal is to alleviate the pressure on emergency departments and fill the gaps in access to basic healthcare after hours.
Khuncho24/shutterstock
Pressure in public hospitals
Pressure in a public hospital has been built for over a decade. Emergency departments are often clogged, which leads to long waiting times, mainly due to personnel deficiencies. About 10% of patients Wait more than two hours. The system has a petite slack to counteract the unpredictable escalate in demand for care.
Since Covid, the percentage of patients with the emergency department has been slow on time. For example, the percentage of patients requiring urgent care in the emergency department, for example decreased from 67% to 61%. More patients who are not subordinate and semiconductor also do not receive time on time.
Patients also wait longer for the planned operation of the Public Hospital since Covid, despite the escalate in the number of admissions from the waiting list for surgical surgical.
Percentage of patients observed on time in emergency departments in a public hospital
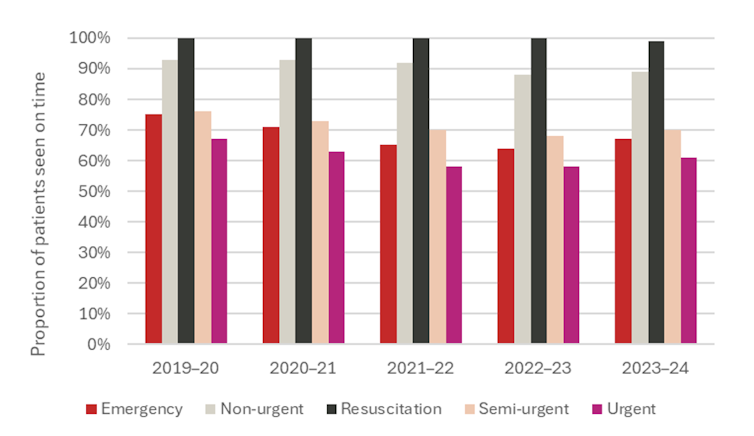
Australian Institute of Health and Social Welfare
Waiting times vary depending on the state and territories. Queensland has lowest percentage Patients waiting for over 365 days for surgery to choose from in a public hospital at the level of 3.9% in 2023–24, while the Act was the highest level of 8.9%.
Encouraging, waiting times decreased for almost all operations to choose from Compared to 2022–23, suggesting that public hospitals can lead to a load on the site.
Percentage of patients waiting for over 365 days for surgery to a public hospital
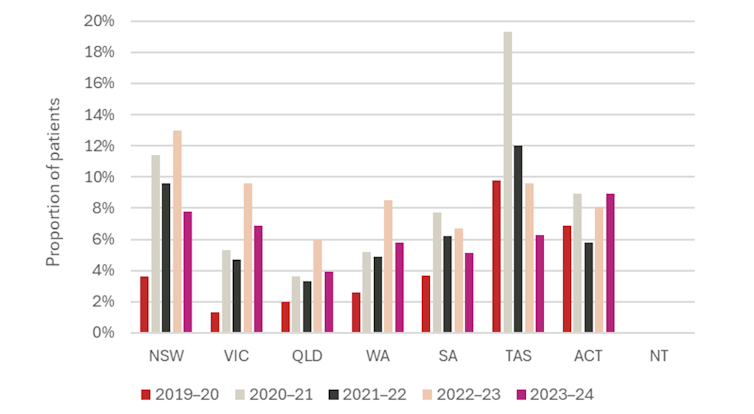
Australian Institute of Health and Social Welfare
Will the money aid?
Although additional financing will aid, there is no magic wand. Public hospitals must significantly reorganize their employees, work flows, beds and buildings. It is in an environment where labor deficiencies lack, burning and Pressure for remunerationA particularly hard escalate in vast changes in the healthcare system.
Some hospitals can significantly reduce the waiting time if the states and territories allocate their additional funds on needy contractors.
Low performance, however, may be associated with system problems without hospital control, such as working strength deficiencies. Without an escalate in the amount of healthcare, these poorly performing hospitals can look for additional staff from other public hospitals, deterioration of their results.
Whether any last improvements is another question.
Public hospitals are facing increased demand for care at the emergency department, only alleviated by the potential success of urgent care clinics.
Read more: urgent care centers Labor are a step in the right direction – but not a panacea
Public hospitals are also in the face of an escalate in the demand for planned surgery, as the population increases and the spread of chronic diseases.
An additional $ 1.7 billion is just one of them. Funds to shorten the waiting time will be spent mainly on a larger number of employees, such as nurses, clinicians and administrative staff.
Public hospitals will need additional current funds to keep up with demand, otherwise every initial improvement will disperse.

Gorodenkoff/Shutterstock
What else has to happen?
All governments must invest more in prevention programs to tardy down the escalate in demand for public hospitals.
More Australians are obese as a percentage of population, compared to other OECD countries. It caused a bulky weight.
The reduction of financial waste in the healthcare system is of great importance. Savings can be used for long -term improvements while waiting, when additional financing ends.
About 40% of healthcare It has a low value or causes damage. A good start is to reduce unnecessary medical examinations, accelerate dumps and reduce admission.
Other changes that may aid:
- Determining the national goals for countries and territories to reduce their waiting lists
- stronger efficiency monitoring
- Conducting managers managers more responsible for achieving the goals of waiting time.
The recent national health reform agreement is to apply in 2026, whoever wins this year’s federal election will have to finalize this agreement with the States and territories.
The community and the countries must still commit to all recommendations from Review of the current contract The degree issued in October 2023 to which governments accept these recommendations can potentially create a much larger, long -term impact on the waiting time than this additional one -time payment.

